Question & Answer - Feeding, Eating, & Drinking
My daughter was born with poor oral motor skills. She had difficulty with both breast and bottle feeding. What should parents know to resolve these problems, as well as possible future feeding and speech issues?QUESTION FROM A MOM ON THE EAST COASTOctober 2013 |
|||
|
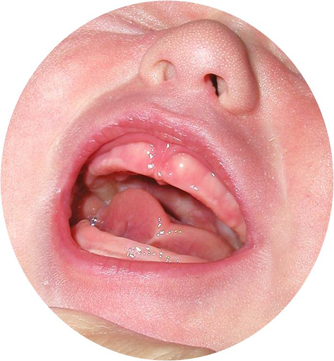
HISTORY: My daughter was born at 39 weeks gestation, weighed 9 pounds, 15 ounces, and was 21.25 inches in length. She had a severe tongue tie that took several attempts to correct surgically. She also had a one-sided jaw weakness as evidenced by a very weak bite reflex on one side. My daughter was unsuccessful with breastfeeding and floundered with bottle feeding. She finally formed a weak seal on the bottle with cheek compression. I also could not feel her sucking pads. However, I was lucky enough to have two excellent feeding specialists (a lactation consultant and a speech-language pathologist) who helped me successfully feed my daughter. Since my daughter had breast and bottle feeding problems, I am concerned that she may have problems with other feeding skills and speech. PHOTO OF ANTERIOR TONGUE TIE PROVIDED BY CATHERINE WATSON GENNA, BS, IBCLC, RLC ANSWER FROM DIANE BAHR, MS, CCC-SLP Thank you for submitting this question. I think many parents experience these types of problems but may not have the professionals available to help them as you did. It sounds like many factors contributed to your daughter’s feeding problem, making it rather complicated. We will discuss each factor and the possible future outcomes below. Near-Term Babies and Sucking Pads Let’s begin by talking about the importance of sucking pads. Despite being a good size and weight, your daughter was a near-term baby (born between 37 and 40 weeks gestation). Sucking pads (also known as cheek pads) develop toward the end of pregnancy when other fat is developing on a baby’s body. They are balls of fat in a baby’s cheeks. When a baby has a full set of sucking pads, you can barely squeeze your finger inside the baby’s cheek areas. Babies need sucking pads to attain adequate pressure in the mouth for suckling and sucking. Here is a video showing how sucking pads and other mouth structures work in the context of breastfeeding. Click on the underlined link for the video. Since your daughter was a near-term baby, she may not have had a full set of sucking pads. I have worked with many near term babies who had mild to moderate feeding problems that seemed related to thin or missing sucking pads. These babies often had difficulties with breastfeeding and tended to do better with bottle feeding. While they seem similar, breast and bottle feeding are actually different processes. Breastfeeding is superior to bottle feeding (if a mother can breastfeed) as the process of breastfeeding supports mouth and airway development in a way that bottle feeding cannot (See Bahr, 2010, pp. 29-31 for a complete explanation). Cheek pads do not develop after birth, so a child (who has thin or missing sucking pads) must learn to use his or her cheek muscles to compensate for the lack of sucking pads. Most babies can be taught to pull the cheeks inward to create the intraoral pressure needed to suckle, suck, and swallow efficiently through activities such as carefully-applied cheek support. In terms of development, sucking pads shrink as a baby begins using the mouth for spoon-feeding, cup and straw drinking, chewing, and other increasingly mature feeding processes (between 4 and 6 months of age). As sucking pads disappear, the cheek muscles replace their function by actively positioning the cheeks against the gums during feeding processes (Bahr, 2010, pp. 48-51). Based on your description, your feeding specialists taught you to use carefully-applied cheek support to assist your daughter with feeding. Cheek support can also help to activate a baby’s lips.
Tongue Tie and Lip Restriction As you know, a newborn’s tongue should be mobile, not tied or restricted. While it took several attempts, you had your daughter’s tongue surgically released. As you learned, a tongue tie can significantly affect a baby’s ability to feed. Several websites contain outstanding information on this topic for parents and professionals (i.e., cwgenna.com, Drjain.com, brianpalmerdds.com, kiddsteeth.com/articles). During feeding, a baby’s tongue needs to move freely in a front-back wavelike motion (with the tongue coming just over the lower gum). Babies with tongue tie often have difficulty with breastfeeding, and many also have difficulty with bottle feeding. Compare the video x-ray of Baby Z with a posterior tongue tie to the x-ray of a child who is bottle feeding normally. Click on the underlined links for the videos. If not corrected, a tongue tie can limit a child’s ability to lift and move his or her tongue throughout the mouth in order to:
Once a child’s tongue tie is released, it is important to monitor these processes as the child develops feeding and speech skills. Tongue tie may be corrected surgically (as you did for your daughter) or through hands-on treatments depending on the degree of restriction. Some therapists know facilitation techniques (which can be taught to parents and caregivers) to help alleviate a mild tongue restriction. Click on the underlined link for the video. Facilitation techniques can also help a child learn to move the tongue appropriately after surgery (once approved by the doctor). Surgery is usually done by an otolaryngologist, oral surgeon, or dentist. In some cases, scar tissue may form under the tongue after surgery, particularly after multiple clippings. Scar tissue can restrict tongue movement. Laser surgery/treatment has been used to resolve scar tissue. While we are discussing tongue restriction, we should also discuss lip restriction. Some children with tongue ties also have lip restrictions. The same type of membrane that connects a baby’s tongue to the floor of the mouth also connects the baby’s upper and lower lips to their respective gums. These membranes are called frenums. Lip restriction may be corrected surgically or through hands-on facilitation techniques. Lip restrictions can inhibit a baby’s lip movements. This problem may affect a baby’s lip flare needed for an effective latch during breast or bottle feeding. In the video of Baby Z (with a posterior tongue tie), the lower lip seems more active than the upper lip, indicating a possible upper lip restriction. Click on the underlined link for the video. As a child grows, lip restrictions may also affect the child’s ability to effectively remove food from a spoon, drink from a cup or straw, and produce speech sounds involving the lips. These are skills you may want to monitor as your daughter develops. Jaw Weakness You mentioned that your daughter’s bite reflex was weak on one side. This type of jaw imbalance may be related to improper positioning within the womb or torticollis. Feeding specialists are seeing a lot of torticollis these days, and torticollis has a relationship to reflux. You did not mention torticollis or reflux. So, your daughter’s jaw imbalance may have been related to her positioning in the womb, since she was a rather large baby. As you know, the phasic bite reflex is stimulated by pressing on a baby’s upper and lower gum surfaces. When you do this, you see and feel an up-down rhythmic munching pattern of approximately one-per-second. It is interesting how many body rhythms occur at one-per-second (e.g., the nutritive suckle, the human heart rate, etc.). You likely did some specific jaw treatment with your daughter to correct the imbalance in her bite response (Bahr, 2010, pp. 136-147). Stimulating a baby’s phasic bite response engages the muscles that raise and lower the baby’s jaw. The bite reflex helps the baby learn to move the jaw in a controlled manner. A baby needs this jaw control for sucking, taking bites of food, chewing, drinking from a cup or straw, and eventually babbling and speaking. I again suggest that you monitor these skills as they develop in your daughter. A baby gains control over the phasic bite reflex between 5 and 9 months of age when he or she is beginning to chew soft foods. The bite reflex seems to disappear (i.e., is integrated into the motor system) between 9 and 12 months of age as a baby eats foods of increasing texture. Keeping Children ON TRACK in Feeding, Speech, and Mouth Development Based on your question, you want to be sure that the problems your daughter experienced with early feeding will not affect later-developing activities involving her mouth. I commend you for your PROACTIVE PARENTING!!!!! In discussing each topic that affected your daughter’s ability to breast and bottle feed, I frequently recommended that you monitor your daughter’s feeding and speech skills as they develop. When parents know what to expect in their child’s development, they can help a child attain expected outcomes and recognize when their child needs help. I wrote the book Nobody Ever Told Me (or My Mother) That! Everything from Bottles and Breathing to Healthy Speech Development (2010) for this very purpose. It is a parent-friendly, easy-to-use resource which contains detailed feeding, speech, and mouth development checklists from birth to 3 years of age and beyond. It has step-by-step instructions for what to do about problems that arise and explains why parents are doing activities to resolve specific problems. There are now Free Parent Book Guides to help parents and professionals quickly navigate the information in the book. If parents cannot help their children with specific feeding, speech, and mouth development problems, then they need professional help (as you obtained for your daughter). Chapter 9 of Nobody Ever Told Me (or My Mother) That! guides parents in finding the professionals they need. Thank you so very much for sharing your daughter’s feeding story with us. I hope that the information provided here will help you and many other parents. Happy Parenting!!!!!!!! References Babyslime. (2011, Oct. 26). Swallow study for baby with posterior tongue tie. http://www.youtube.com/watch?v=lrD9cemJNyw Bahr, D. Nobody ever told me (or my mother) that! Everything from bottles and breathing to healthy speech development. Arlington, TX: Sensory World. Jain, E. (n.d.). Anterior and posterior tongue tie. http://www.drjain.com/ Genna, C. W. (n.d.). Tongue tie identification. http://www.cwgenna.com/quickhelp.html Kotlow, L. A. (n.d.). Kid’s teeth articles. http://www.kiddsteeth.com/articles.html Palmer, B. (n.d.). For better health. http://brianpalmerdds.com/ Shaw, L. (n.d.). Torticollis and Sandifer’s syndrome. Pollywog: Practical Solutions for Infant Reflux & Colic. http://www.pollywogbaby.com/torticollis-sandifers-syndrome.html SpringerVideos. (2010, Nov. 27). Current practice in paediatric videofluoroscopy. http://www.youtube.com/watch?v=BsfA31hKev0 Tempest Beauty. (2013, May 16). Tongue exercises – Part 1. http://www.youtube.com/watch?v=nhPqXWyPHO4 YouBeauty. (2012, May 3). A newborn’s anatomy aids in breastfeeding. http://www.youtube.com/watch?v=LyE9bVRhW54 |
|||